Malignant Brain Tumor (Glioblastoma)
Disease Description
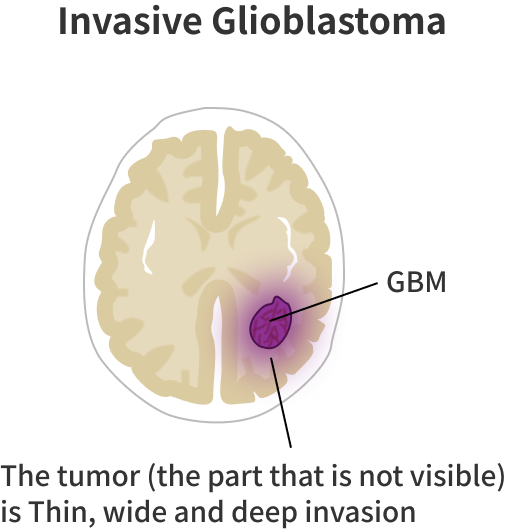
Glioblastoma, which accounts for about half of all primary malignant brain tumors (gliomas), is an extremely malignant disease with a 5-year survival rate of 6.9% and an average survival time of 8 months (National Brain Tumor Society). It is estimated that more than 10,000 people are affected annually in the United States. Glioblastoma is characterized by rapid growth and diffuse invasion into the brain parenchyma.
Current Therapy
Standard therapies include surgery, radiation therapy, and chemotherapy with the anticancer agents temozolomide and the molecularly targeted agent bevacizumab. However, there are few proven effective treatments for patients who have recurred after standard therapy, and there are no treatment options available.
Surgical removal of glioblastoma is difficult because it is hard to visually distinguish from normal tissue and because the tumor is deeply invasive within the brain parenchyma. 3-year survival rate is only 10% even after 100% removal of MRI contrast-enhanced lesions.
The disease is also resistant to radiotherapy.
In chemotherapy, the number of anticancer agents that can reach the brain is limited due to the presence of the blood-brain barrier. At present, few anticancer agents have been shown to be effective. Even when anticancer agents are administered directly into the brain, it is a challenge to deliver them to glioblastoma, which invades deep into the brain.
Our therapeutic approach
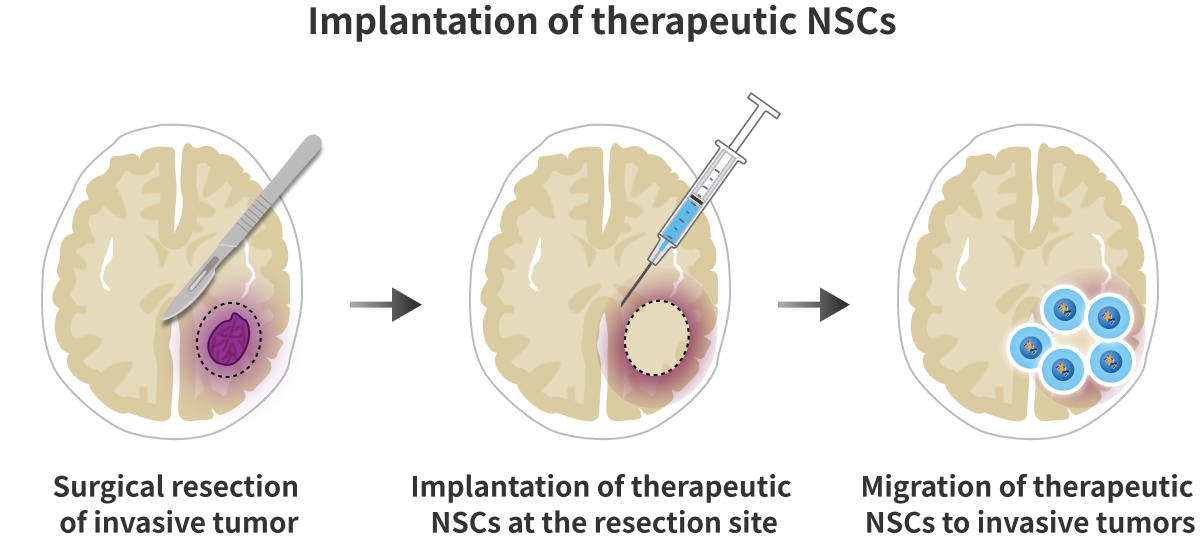
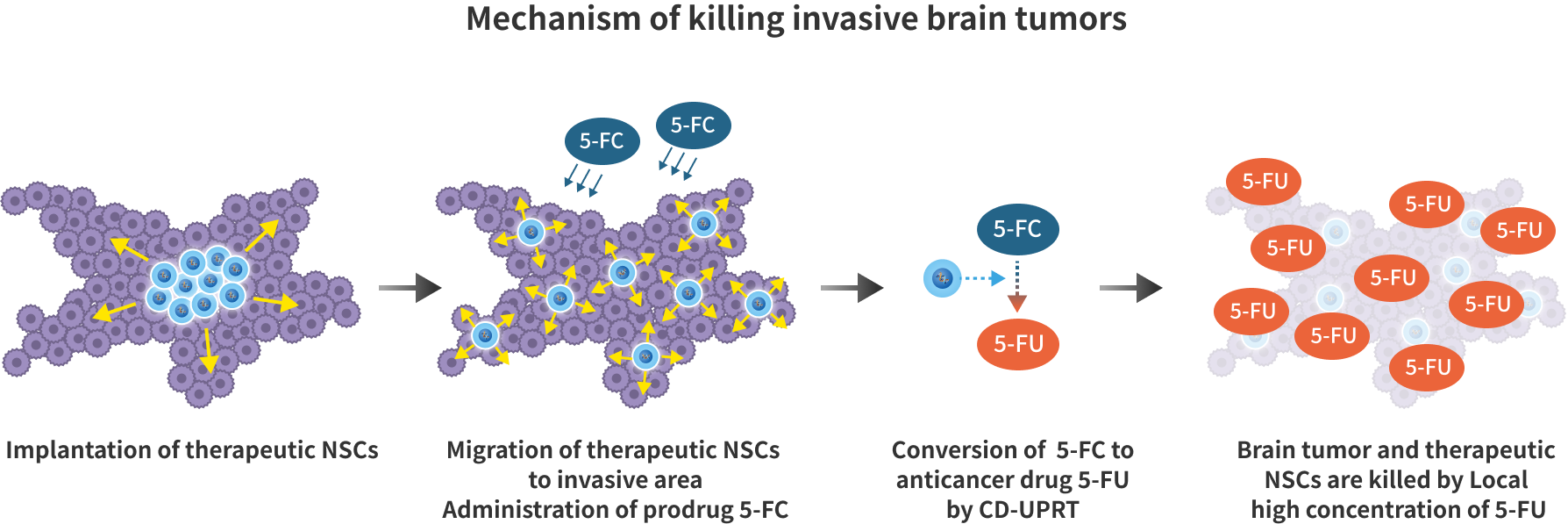
We are developing a novel gene cell therapy for recurrent glioblastoma for which no existing treatment exists.After surgical resection of the recurrent glioblastoma, therapeutic cells (therapeutic NSCs) are implanted directly into the resection site. The implanted therapeutic NSCs sense chemokines released by the tumor and migrate toward the tumor to deliver the therapeutic gene to the glioblastoma vicinity. The prodrug 5-FC then passes through the blood-brain barrier and is converted to the anticancer drug 5-FU only at the tumor site where the therapeutic gene CD-UPRT is present. The high concentration of anticancer drug produced at the tumor site then kills the surrounding glioblastoma.
Since the anti-cancer drug produced is only localized, it is expected to be safer than standard anti-cancer therapies. After its efficacy is proven in recurrent glioblastoma, we are planning to expand its application to primary glioblastoma.